Michigan Lawyers Handling Cases Related to Hypoxic Ischemic Encephalopathy (HIE) and Uterine Rupture
While hundreds of newborns will sustain permanent injuries and disabilities from hypoxic ischemic encephalopathy (HIE) and uterine rupture from medical malpractice this year alone, few will ever obtain any legal help or compensation. At Michigan Cerebral Palsy Attorneys, we aim to educate and empower the families affected by medical malpractice and encourage them to pursue the legal action necessary to secure funds for health care, rehabilitation, and lifestyle supports.
Throughout this page, we’ll discuss how uterine rupture can cause hypoxic ischemic encephalopathy (HIE) and review a few instances of medical malpractice that may entitle patients to compensation. If your loved one suffers from a permanent injury or disability related to a traumatic birth, we encourage you to reach out to our Michigan birth trauma and medical malpractice lawyers today. With nearly fifty collective years of experience solely focusing on birth injury cases, our lawyers have the specific skill and knowledge necessary to win cases related to birth asphyxia, cerebral palsy (CP), infant brain damage, and other birth injuries.
If at any point you have cause inquiries or questions, please do not hesitate to reach out to our Michigan birth injury, hypoxic ischemic encephalopathy (HIE) and uterine rupture lawyers. You may call us toll-free at (888) 592-1857, fill out this online contact form, or press the following button. Our Michigan HIE lawyers are available 24/7 and will provide you with a free case review.
Uterine Rupture and Vaginal Birth after Cesarean (VBAC) Deliveries
Uterine rupture is a serious labor and delivery emergency that can be life threatening for the mother and/or the infant. Typically caused by the strong contractions and forces associated with vaginal delivery, uterine rupture occurs when the uterus tears open. Tearing of the womb may expel the unborn baby into the mother’s abdomen and/or lead to maternal hemorrhaging, both of which are known causes of fetal oxygen deprivation and hypoxic ischemic encephalopathy.
Uterine rupture can be caused by post term labor, the use of labor-induction drugs, abnormal fetal presentation, or multiple gestations, but uterine rupture is most commonly caused by attempting to deliver vaginally after a previous C-section delivery. Women electing Vaginal Birth after Cesarean (VBAC) deliveries are at a greater risk for uterine rupture because scarring around the uterus and/or abdomen (as from a previous C-section scar) weakens the tissues and muscles necessary to withstand the extreme forces of labor and delivery.
Because uterine rupture poses such a great risk to women with previous C-section operations, the American Congress of Obstetricians and Gynecologists (ACOG) stresses that VBAC only be used in carefully chosen, very low risk cases. According to the standards of care, expectant mothers must give clear informed consent to medical professionals before opting to delivery vaginally after a previous C-section. Additionally, medical professionals must determine all potential maternal risk factors for uterine rupture. Read on to learn more about the causes and risk factors for uterine rupture.
Causes and Risk Factors for Uterine Rupture
Because of the severe complications associated with uterine rupture, medical professionals are required to determine whether the mother has any of the following causes or risk factors for uterine rupture before making an informed decision to go through with the delivery.
- Uterine scarring
- Uterine perforation scar
- A single layer closure in a previous C-section
- Scar from a previous C-section delivery
- A hysterectomy scar (these are incisions made during C-section operations for shoulder dystocia)
- Metroplasty or myomectomy scar
- Past trauma (for example, from a previous wound or accident)
- Vaginal Birth after Cesarean (VBAC) delivery
- The use of labor-induction drugs (such as Pitocin or Cytotec)
- Obesity
- The misuse of vacuum extractors or forceps
- Fetal malpresentation (such as breech, shoulder, or face presentation)
- Cephalopelvic disproportion (CPD)
- Black/African American race
- Post-term pregnancy
- A previous delivery that suggests the mother tolerates labor poorly (and thus increases the chance of fetal distress)
- Previous uterine rupture
- A fetus that is large for his or her gestational age (LGA)
- Multiple gestations
Signs of Uterine Rupture
There are a few signs that indicate an increased chance of uterine rupture during vaginal delivery. If any signs of uterine rupture appear, medical professionals must prepare for a fast delivery (usually by Cesarean section). One or more of the following signs should indicate uterine rupture in a mother delivering vaginally after a previous C-section:
- Abrupt abdominal pain and/or abdominal pain that becomes worse
- Vaginal bleeding
- Hemodynamic instability (unstable blood pressure or cardiac output)
- Diminished uterine contractions
- Abnormal fetal heart tracings*
- Baby receding back into the birth canal
*Non-reassuring fetal heart tracings are the most common sign of uterine rupture and indicate the need for an emergency C-section. Experts agree that an emergency Cesarean section operation should be held within eighteen minutes of the uterine rupture in order to prevent the possibility of hypoxic ischemic encephalopathy and permanent infant brain damage.
Hypoxic Ischemic Encephalopathy (HIE) and Uterine Rupture
What is Hypoxic Ischemic Encephalopathy?
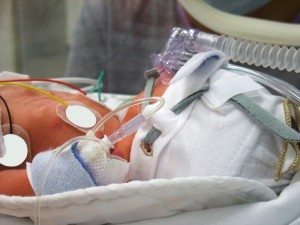 Hypoxic ischemic encephalopathy, also known as neonatal encephalopathy (NE) or birth asphyxia, is a dangerous neonatal brain injury. Hypoxic ischemic encephalopathy is caused by a shortage of oxygen and blood flow to the brain around the time of labor and delivery and can lead to serious, permanent injuries and disabilities including cerebral palsy (CP), periventricular leukomalacia (PVL), neurodevelopmental impairments, learning disabilities, seizure disorders, intellectual and developmental disabilities (I/DD), and more. Depending on the duration and severity of the oxygen-depriving insult, hypoxic ischemic encephalopathy can even lead to fetal demise.
Hypoxic ischemic encephalopathy, also known as neonatal encephalopathy (NE) or birth asphyxia, is a dangerous neonatal brain injury. Hypoxic ischemic encephalopathy is caused by a shortage of oxygen and blood flow to the brain around the time of labor and delivery and can lead to serious, permanent injuries and disabilities including cerebral palsy (CP), periventricular leukomalacia (PVL), neurodevelopmental impairments, learning disabilities, seizure disorders, intellectual and developmental disabilities (I/DD), and more. Depending on the duration and severity of the oxygen-depriving insult, hypoxic ischemic encephalopathy can even lead to fetal demise.
How Can Uterine Rupture Cause HIE?
As mentioned above, hypoxic ischemic encephalopathy is caused by fetal oxygen deprivation around the time of delivery. Hypoxia refers to an oxygen shortage in fetus’ bodily tissues and ischemia refers to restricted blood flow to the fetus and the fetus’ brain. Uterine rupture can cause hypoxic ischemic encephalopathy in the following ways:
- Maternal blood loss: Uterine rupture often causes rapid, uncontrolled blood loss (hemorrhaging) in the mother, which ultimately significantly decreases the amount of oxygenated blood reaching the fetus. Additionally, maternal hemorrhaging may cause the mother to go into shock and experience abnormally low blood pressure, which is life threatening for the fetus.
- Placental abruption: Uterine rupture can cause placental abruption, a labor and delivery emergency in which the placenta separates from the uterine wall. Placental abruption dangerously interferes with the passage of oxygenated blood from the placenta to the baby, ultimately diminishing oxygen levels in the baby’s brain.
- Umbilical cord problems: After a uterine rupture, the baby may potentially move out of the uterus and into the mother’s abdomen. When this happens, the umbilical cord may stretch, tear, or become compressed, thereby interfering with the passage of oxygenated blood from the mother to the fetus.
The most extreme form of hypoxic ischemic encephalopathy (HIE) is known as anoxia, or complete, prolonged oxygen deprivation. It is the most common form of birth asphyxia in cases of uterine rupture, and often causes fetal death.
Uterine Rupture, Hypoxic Ischemic Encephalopathy (HIE), and Medical Malpractice
Michigan Birth Injury Lawyers Representing Victims of Medical Malpractice with Hypoxic Ischemic Encephalopathy (HIE) and Uterine Rupture Injuries
Pursuing legal action for your uterine rupture and hypoxic ischemic encephalopathy (HIE) case is the first step towards securing a better life for your family. When seeking legal help for a complicated birth injury case, it is crucial to find a lawyer and law firm with specific and extensive experience. At Michigan Cerebral Palsy Attorneys, our birth asphyxia lawyers have secured compensation for numerous Michigan families affected by birth injuries including hypoxic ischemic encephalopathy (HIE) and uterine rupture.
Uterine rupture can lead to hypoxic ischemic encephalopathy in a few instances of medical malpractice. For example, the following medical mistakes may cause HIE:
- The failure of a medical professional to monitor the mother and the baby during labor and delivery
- The failure of a medical professional to test for and determine risk factors for uterine rupture
- The failure of a medical professional to detect signs of uterine rupture
- The failure of a medical professional to quickly deliver the baby and/or call for a timely emergency C-section
If your loved one was diagnosed with a birth injury or disability such as cerebral palsy, hypoxic ischemic encephalopathy (HIE), or a seizure disorder, contact our Michigan birth injury attorneys today. The award-winning lawyers from our birth injury law firm will provide you with a free case review, answer your questions, and discuss your legal options with you. Should we take your case, our no-fee policy ensures you will not be charged unless we win or settle in your favor. Hypoxic ischemic encephalopathy (HIE) and uterine rupture are dangerous, life-altering birth injuries and our Michigan medical malpractice attorneys are committed to fighting for the compensation you deserve. Contact Michigan Cerebral Palsy Attorneys in any of the following ways—
Complete our quick online contact form here
Call us toll-free at (888) 592-1857
Related Reading
More information about birth injuries, Michigan Cerebral Palsy Attorneys, hypoxic ischemic encephalopathy (HIE) and uterine rupture:
- Hypoxic Ischemic Encephalopathy (HIE) and Uterine Rupture
- Uterine Rupture
- Hypoxic Ischemic Encephalopathy
- Hypoxic Ischemic Encephalopathy Infographic
- Hypothermia Treatment for Hypoxic Ischemic Encephalopathy
- Hypoxic Ischemic Encephalopathy (HIE) and Nuchal Cords
- Hypoxic Ischemic Encephalopathy (HIE) and Seizures
- Hypoxic Ischemic Encephalopathy (HIE) in Twins and Multiples
- Hypoxic Ischemic Encephalopathy (HIE) from the Misuse of Pitocin & Cytotec
- HIE, Uterine Rupture, and the Law
- Blogs
