What Is Villitis?
Villitis is a serious maternal health complication that occurs when a placental infection is left untreated. Villitis is characterized by the inflammation of the placenta’s chorionic villi surface, which is the area of the placenta responsible for nutrient, blood, and gas exchange between the mother and fetus. Villitis greatly increases the chances of fetal death, so it is crucial for physicians to immediately diagnose and treat certain infections and risk factors that can lead to villitis.
Since villitis generally develops as a result of severe or untreated maternal infection, its presence often signifies medical negligence. If your child’s cerebral palsy (CP) or lifelong injury occurred as the result of untreated villitis, call our experienced Michigan cerebral palsy lawyers today. Legal and medical professionals from our team will review your case for free and inform you of your legal options. Our Michigan cerebral palsy attorneys are available to speak with you 24/7. Contact Michigan Cerebral Palsy Attorneys in any of the following ways:
Contact our lawyers online by filling out this quick form
Call Michigan Cerebral Palsy Attorneys toll-free at (888) 592-1857
Live Chat with our attorneys by pressing the tab to the left
What Causes Villitis?
The exact cause of villitis is unknown, but the condition is associated with different placental infections (commonly chorioamnionitis). Experts speculate that the following bacterial and viral conditions cause villitis:
- Bacterial causes of villitis:
- Chorioamnionitis: Intra-amniotic infection caused by vaginal bacteria ascending into the uterus
- Streptococci bacteria
- Maternal sepsis bacteria: Maternal sepsis is a severe blood infection in which a pregnant woman’s body reacts to a certain bacterial infection.
- Syphilis: A sexually transmitted bacteria that may cause premature birth, stillbirth, and developmental issues.
- Viral causes of villitis:
- Cytomegalovirus (CMV): CMV is a viral infection spread through bodily fluids. Mothers can pass CMV to a newborn through breast milk.
- Taxoplasmosis, which is a parasitic disease mothers can pass to their babies.
- Herpes: Babies can come in contact with herpes in the womb or birth canal
- Rubella: More commonly known as German measles, pregnant women can pass rubella to their babies in the womb.
What Injuries Result from Villitis?
- Hypoxia (severe limitation in the baby’s oxygen supply)
- Hydrops fetalis (abnormal fluid build-up in two or more areas of a fetus)
- Intrauterine growth restriction (IUGR) (small baby): Villitis leads to smaller than average babies because of the poor nutrient and oxygen transfer to the baby
- Premature rupture of the membranes (PROM): Villitis may cause the mother’s water to break more than one hour before labor begins.
- Preterm birth
- Respiratory problems
- Meningitis or other bacterial infections
- Encephalopathy (brain injury, such as hypoxic ischemic encephalopathy)
- Brain damage, such as cerebral palsy and periventricular leukomalacia (PVL)
- Neonatal sepsis (blood infection)
- Fetal death/stillbirth
What Are the Risk Factors for Villitis?
- Viral, bacterial, and protozoal infections
- Obesity during pregnancy
- Multiple births (the mother is pregnant with more than one baby)
- Urinary complications during pregnancy
What Are the Signs and Symptoms of Villitis?
- Chronic villitis:
- Elevated levels of alpha-feto-protein when intrauterine growth restrictions (small babies) are present
- Non-significant elevations of human growth hormone when testing for abnormal number of chromosomes in the second trimester.
- Acute villitis
- Abscesses in the placental parenchyma (villi)
- Chorioamnionitis
How Is Villitis Diagnosed and Treated?
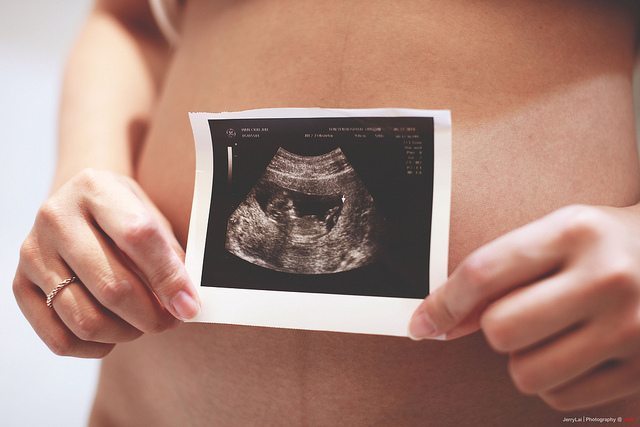 Villitis is difficult to detect without a microscope, and thus it often goes undiagnosed. The only way to spot villitis is by identifying an abscess formation with an ultrasound reading.
Villitis is difficult to detect without a microscope, and thus it often goes undiagnosed. The only way to spot villitis is by identifying an abscess formation with an ultrasound reading.
However, since villitis is associated with placental infections, physicians should be on the lookout for villitis if any of the following conditions are present:
- CMV (Cytomegalovirus)
- Chorioamnionitis
- Candida, which is a type of yeast infection
- HSV
- Group B Streptococcus
- Group A Streptococcus
- Syphilis
- Toxoplasmosis
- Chlamydia
The patient should immediately begin steroid and aspirin regimens after villitis is diagnosed.
Legal Help for Villitis and Cerebral Palsy
Physicians are obligated to monitor both the mother and the fetus particularly closely when the risk factors for villitis are present. Listed below are incidents that may constitute as negligence in villitis cases:
- Failure to diagnose and treat the risk factors for villitis (placental infection, ascending infections, etc.)
- Failure to closely monitor the mother and child when infection is present
- Failure to obtain informed consent, which includes information about alternative delivery methods and risks associated with villitis
To find out if your child is eligible for compensation due to an improperly treated infection that led to villitis, contact our skilled Michigan birth injury attorneys. You may call our offices toll-free at (888) 592-1857, fill out this online contact form, or press the Live Chat tab to the left.
Sources:
- Cornette L. Fetal and neonatal inflammatory response and adverse outcome. Semin Fetal Neonatal Med 2004; 9:459.
- Lieberman E, Lang J, Richardson DK, et al. Intrapartum maternal fever and neonatal outcome. Pediatrics 2000; 105:8.
- Soper DE, Mayhall CG, Dalton HP. Risk factors for intraamniotic infection: a prospective epidemiologic study. Am J Obstet Gynecol 1989; 161:562.
- Frigoletto FD Jr, Lieberman E, Lang JM, et al. A clinical trial of active management of labor. N Engl J Med 1995; 333:745.
- Newton ER. Chorioamnionitis and intraamniotic infection. Clin Obstet Gynecol 1993; 36:795.
- Yoon BH, Romero R, Moon JB, et al. Clinical significance of intra-amniotic inflammation in patients with preterm labor and intact membranes. Am J Obstet Gynecol 2001; 185:1130.
- Rouse DJ, Landon M, Leveno KJ, et al. The Maternal-Fetal Medicine Units cesarean registry: chorioamnionitis at term and its duration-relationship to outcomes. Am J Obstet Gynecol 2004; 191:211.
- Kradin, RL. Perinatal Infections. In: Diagnostic Pathology of Infectious Disease: Expert Consult, Saunders, 2010. p.465.
