What Is Oligohydramnios?
Oligohydramnios is a pregnancy condition characterized by a shortage of amniotic fluid. Amniotic fluid is the liquid in the amniotic sac that encapsulates and protects the baby during pregnancy. By breathing and swallowing the amniotic fluid, the baby receives the nutrients necessary for healthy lung maturation, growth, and temperature. Understandably, a shortage of amniotic fluid can result in severe developmental consequences, secondary pregnancy complications, and fetal and maternal injuries.
Do you believe oligohydramnios caused your loved one’s cerebral palsy or lifelong injury? If so, you may have grounds for a medical malpractice or personal injury claim. We encourage you to contact our experienced Michigan cerebral palsy lawyers to learn about your legal options today. Our birth injury lawyers will evaluate your birth injury case for free. Should Michigan Cerebral Palsy Attorneys take your case, you will not be charged until we win or settle in your favor. You may reach our Michigan cerebral palsy and birth injury lawyers in whichever way best suits you:
Call us toll-free at (888) 592-1857
Live Chat with our attorneys by clicking the Live Chat tab on the left
Fill out this online contact form
What Causes Oligohydramnios?
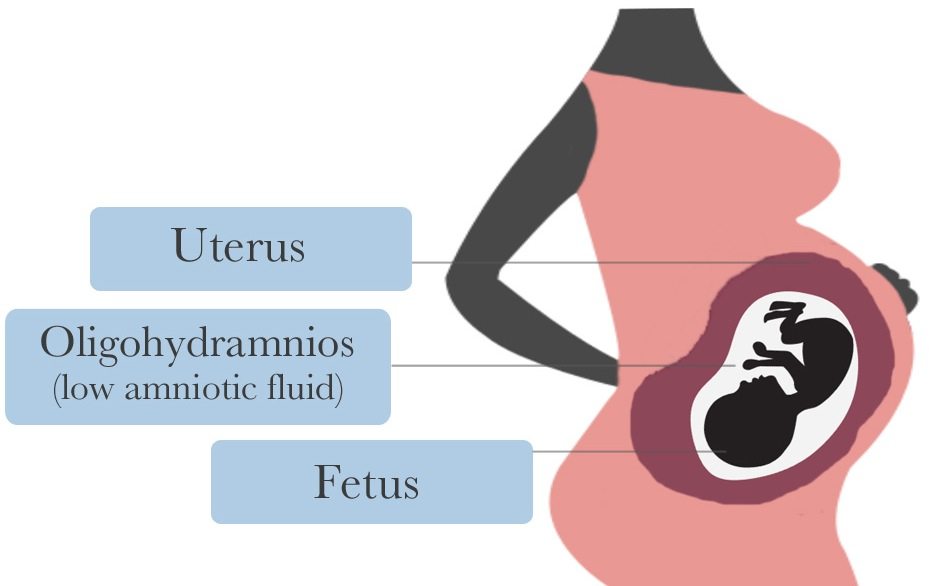 Amniotic fluid levels are determined by the amount of fluid flowing in and out of the amniotic sac. There are a number of potential causes for reductions in amniotic fluid levels, which we’ve categorized into the following groups: maternal causes, placental causes, and fetal causes.
Amniotic fluid levels are determined by the amount of fluid flowing in and out of the amniotic sac. There are a number of potential causes for reductions in amniotic fluid levels, which we’ve categorized into the following groups: maternal causes, placental causes, and fetal causes.
A. Maternal Causes
- Preeclampsia (pregnancy-induced high blood pressure)
- Diabetes, gestational diabetes, or kidney disease
- Dehydration
- High blood pressure medications
- Chronic hypertension (high blood pressure)
- Collagen vascular disease (connective tissue disease)
B. Placental Causes
- Placental abruption
- Placental thrombosis/infarction (clots or obstructed placenta blood flow)
- Uteroplacental insufficiency (placenta not functioning adequately)
- Twin to twin transfusion syndrome (the shared placenta of identical twins contains abnormal blood vessels and insufficient nutrients for both babies)
C. Fetal Causes
- Growth restriction: A growth restricted fetus may redistribute blood flow away from the kidneys, which decreases fetal urine production and causes oligohydramnios.
- Gastrointestinal abnormalities that block the passage of fluid.
- Fetal demise
- Post term pregnancy: Numerous complications can occur when a baby is post term, such as placental insufficiency and a macrosomic (large) baby.
- Premature rupture of the membranes (PROM)
- Congenital abnormalities, particularly those associated with impaired urine production, which occurs when there are problems with the baby’s kidneys.
- Chromosomal abnormalities such as Down’s syndrome or an abnormality that causes problems with swallowing.
- Absence of fetal urine production
What Are the Risk Factors for Oligohydramnios?
Since many pregnant women with oligohydramnios don’t have any identifiable risk factors, physicians should closely monitor a woman’s amniotic fluid levels during pregnancy. Some risk factors that predispose pregnant women to oligohydramnios include:
- Maternal hypertension (high blood pressure), including preeclampsia (pregnancy-induced hypertension)
- Maternal diabetes: Including preexisting diabetes or pregnancy-induced diabetes (gestational diabetes)
- Placental problems
- Lupus
What Are the Signs and Symptoms of Oligohydramnios?
- Rapid growth of the uterus
- Discomfort in the abdomen
- Leaking amniotic fluid
- Little to no fetal movement inside the womb
- Uterine contractions
How Is Oligohydramnios Diagnosed?
 Doctors diagnose oligohydramnios with physical exams, health history assessments, and ultrasound readings. During oligohydramnios diagnosis, doctors use ultrasound readings to gather amniotic fluid level measurements and calculate a woman’s “AFI” (amniotic fluid index) to determine if her levels are normal. Throughout the pregnancy, doctors should regularly reevaluate a woman’s AFI and measure fetal heart rate, breathing, movements, and muscle tone to assess fetal well being.
Doctors diagnose oligohydramnios with physical exams, health history assessments, and ultrasound readings. During oligohydramnios diagnosis, doctors use ultrasound readings to gather amniotic fluid level measurements and calculate a woman’s “AFI” (amniotic fluid index) to determine if her levels are normal. Throughout the pregnancy, doctors should regularly reevaluate a woman’s AFI and measure fetal heart rate, breathing, movements, and muscle tone to assess fetal well being.
Oligohydramnios affects 4 – 8 % of pregnancies and needs to be diagnosed and managed early to prevent fetal injury. With early diagnosis, most cases of oligohydramnios can be managed or treated with hospital bed rest, fetal monitoring, oral and intravenous hydration, and early delivery when the fetal monitor shows abnormal heart rates.
How Is Oligohydramnios Treated?
While there is no long-term treatment for oligohydramnios, drinking extra fluids, installing a saline solution into the amniotic sac (amniofusion), and other intravenous fluid delivery procedures have been proven to increase amniotic fluid levels.
The management options for oligohydramnios greatly depends on the trimester in which the condition arises—presence of oligohydramnios in the first trimester usually results in fetal death while occurrence of the condition later in the pregnancy offers more promising outcomes. Physicians should assess the short and long term fetal risks of oligohydramnios at each prenatal visit, monitor fetal heart rate closely, and measure other factors of fetal well being . If fetal heart rate abnormalities occur, physicians should induce labor.
Legal Help for Oligohydramnios Injury and Cerebral Palsy (CP)
Injuries associated with oligohydramnios are complex and devastating, so it is important for physicians to follow the medical standards of care and carefully monitor the mother and baby throughout the pregnancy.
Negligent incidents include the following:
- Failure to thoroughly assess the mother’s health history, thereby failing to recognize risk factors for oligohydramnios
- Failure to inform the mother about the risks, benefits and alternatives to management plans for oligohydramnios and delivery
- Failure to carefully monitor the mother and baby during pregnancy and identify low amniotic fluid, diminishing amniotic fluid, placental insufficiency, fetal distress and oligohydramnios risk factors
- Failure to prevent or treat conditions that may cause oligohydramnios, such as gestational diabetes, dehydration, or hypertension
- Improper use of delivery assistance tools (forceps and vacuum extractors)
- Failure to follow standards of care and deliver the baby in a timely fashion; failure to order a C-section; failure to follow standards for late preterm delivery and deliver the baby between 36-37 gestational weeks in cases of isolated and persistent oligohydramnios
You don’t have to confront the medical and emotional burdens of your child’s cerebral palsy alone. Contact our nationally recognized Michigan cerebral palsy attorneys at (888) 592-1857 today for a free evaluation of your case.
Sources:
- Locatelli A, Zagarella A, Toso L, et al. Serial assessment of amniotic fluid index in uncomplicated term pregnancies: prognostic value of amniotic fluid reduction. J Matern Fetal Neonatal Med 2004; 15:233.
- Rutherford SE, Phelan JP, Smith CV, Jacobs N. The four-quadrant assessment of amniotic fluid volume: an adjunct to antepartum fetal heart rate testing. Obstet Gynecol 1987; 70:353.
- Sarno AP Jr, Ahn MO, Brar HS, et al. Intrapartum Doppler velocimetry, amniotic fluid volume, and fetal heart rate as predictors of subsequent fetal distress. I. An initial report. Am J Obstet Gynecol 1989; 161:1508.
- Mercer LJ, Brown LG, Petres RE, Messer RH. A survey of pregnancies complicated by decreased amniotic fluid. Am J Obstet Gynecol 1984; 149:355.
- Yoshimura S, Masuzaki H, Gotoh H, Ishimaru T. Fetal redistribution of blood flow and amniotic fluid volume in growth-retarded fetuses. Early Hum Dev 1997; 47:297.
- Underwood MA, Gilbert WM, Sherman MP. Amniotic fluid: not just fetal urine anymore. J Perinatol 2005; 25:341.
